Welcome Home
Bandage Changes Promote Healing
While your health care provider puts that first bandage on you at the hospital, it’s up to you to change that bandage at least 2x a day, or as directed by your doctor, to help keep your wound clean.1 Yesterday’s bandage may collect bacteria that can cause infection and may not optimally absorb excess wound exudate if it’s reached its capacity. That’s why it’s important to put on a clean bandage every time you remove one. Never apply a new bandage on top of an old one.
7 Simple Steps
Step 1: Place all your wound care items on a sterile surface mat to keep them clean.
NURSE TIP: Make sure you pre-cut your tape or wrap before you start. This makes it easier to put your bandage on.
Step 2: Make sure to wash and dry your hands thoroughly2. Put on your disposable gloves. This lowers the chance of contaminating your wound.
Step 3: Carefully remove your bandage from your skin. You can use saline water to loosen it if it’s hard to remove.
Step 4: Clean your wound gently with a wet gauze pad or gauze sponge. Make sure your wound is completely cleaned of blood and other fluids.
NURSE TIP: When using a gauze pad or a sponge to clean your wound, keep them in the wrapper as you wet it with saline. The less you handle them, the more sterile they will be.
Step 5: After the wound is dry, gently apply your treatment ointment to the wound.
Step 6: Apply a clean non-stick pad or gauze pad to cover your wound. If needed, you can apply extra gauze for extra cushioning.
CLEAN your wound at least 2x a day, as directed by doctor, or as needed when blood or wound exudate has leaked through the bandage.
Step 7: Secure the new, clean bandage in place with tape or wrap. If using tape, carefully apply it to two or more edges of the bandage. If using a wrap, wrap it around the bandage firmly, but not too tight. Make sure it feels comfortable to you.
You may notice your wound draining more heavily in the early days of healing. This is usually a normal part of the healing process. If you experience excessive drainage for a prolonged period of time or drainage that that has an off odour or colour, contact your doctor. You can use the chart below to find the product that has the absorbency you need. If your bandage becomes soaked through at any time, make sure to replace it with a clean, dry bandage. Remember to change your bandage at least 2x a day, or as directed by your doctor, to help keep the wound clean.1
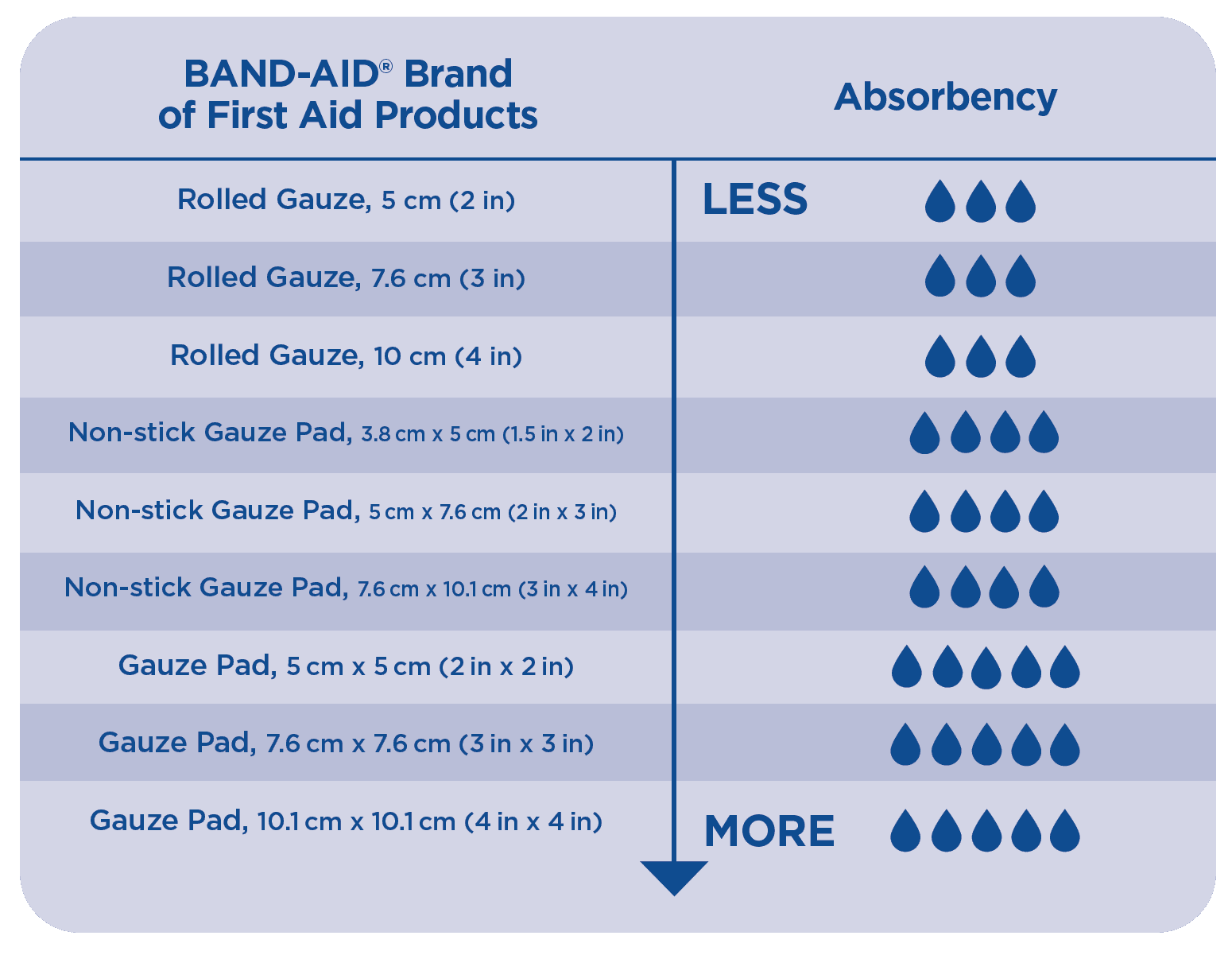
| BAND-AID® of First Aid Products | Absorbency |
|---|---|
| Rolled Gouze, 5 cm (2 in) | LESS 3 |
| Rolled Gauze, 7.6 cm (3 in) | 3 |
| Rolled Gauze, 10 cm (4in) | 3 |
| Non-stick Gauze Pad, 3.8 cm x 5 cm (1.5 in x 2 in) | 4 |
| Non-stick Gauze Pad, 5 cm x 7.6 cm (2 in x 3 in) | 4 |
| Non-stick Gauze Pad, 7.6 cm x 7.6 cm (2 in x 3 in) | 4 |
| Gauze Pad, 5 cm x 5 cm (3 in x 3 in) | 5 |
| Gauze Pad, 7.6 cm x 7.6 cm (3 in x 3 in) | 5 |
| Gauze Pad, 10.1 cm x 10.1 cm (4 in x 4 in) | MORE 5 |
*1, 2, 3, 4 and 5 droplet ratings represent 0, 0-0.15, 0.16-0.3, 0.31-0.45, 0.46-0.6 g/cm2 of fluid absorbency, respectively. Rating for rolled gauzes assumes 2-ply application.
References:
- Cuts and scrapes: first aid. Mayo Clinic Web site. http://www.mayoclinic.org/first-aid/first-aid-cuts/basics/art-20056711. Accessed March 14, 2014.
- Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR; Hospital Infection Control Practices Advisory Committee. Guideline for prevention of surgical site infection, 1999. Infect Control Hosp Epidemiol. 1999;20(4):247-278.


